Chemical signals are transmitted between brain cells by neurotransmitters, which are chemical signals. They have an impact on mood, memory, cognitive performance, and appetite. This blog explores how neurotransmitters function in the brain, as well as what happens when they aren’t functioning properly. It also covers a variety of neurotransmitters and their pharmacological treatments. By learning about the elements, you’ll be able to better understand how your emotions and ideas are managed.
What is a neurotransmitter?
For brain function, the neurotransmitters are required. These are substances that assist in the transmission of information between neurons. This communication is important for a variety of reasons, including memory formation and consolidation. Understanding how neurotransmitters work is critical if you want to better comprehend your own mental health. Certain cognitive operations, such as memory formation and consolidation, are controlled by neurotransmitters. Knowing this may help you manage stress and anxiety more effectively by improving your thinking clarity.
Types of Neurotransmitters
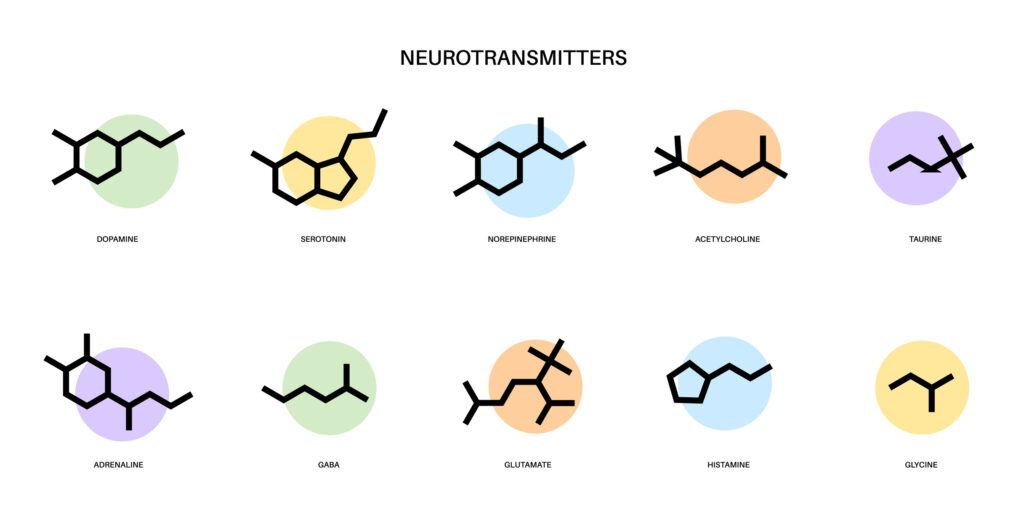
In the brain, neurotransmitters play a key role. Learning and memory are aided by them, and when they are insufficient, it may cause anxiety, depression, addiction, or idiopathic scoliosis. Fortunately, neurotransmitters come in three categories: excitatory, inhibitory, and modulating, each with its own function in brain activity. You may start to address the root of the issue by understanding which neurotransmitter is out of whack. It’s critical to maintain neurotransmitter levels in check by eating a healthy diet and exercising on a regular basis to avoid these symptoms. In addition, keeping neurotransmitter levels in check is possible through a healthy lifestyle.
Neurotransmitters and Scoliosis
In the brain and spinal cord, neurotransmitters are critical. Postural control and long-term muscle memory patterns are impacted by these. Scoliosis unfortunately has no cure at this time, although treatments that address the root causes may help reduce scoliosis over time. Neurotransmitters are tiny chemicals that transmit signals between cells by binding to receptors. Since they may pass via the blood-brain barrier, they are neurotransmitters. Their role in the development of nervous system function and their role in the regulation of neurotransmitter levels are just two reasons why neurotransmitters are critical. Certain neurotransmitters, mainly owing to their influence on muscle memory, muscle coordination, and autoregulation of brain neurotransmitter levels, have recently been linked to idiopathic scoliosis.
Serotonin
Serotonin has a significant impact on mood and emotions. The brain, platelets, and gastrointestinal system have the highest concentrations. Serotonin deficiencies could cause scoliosis, among other things. Serotonin is produced in the highest amounts by the brain, platelets, and gastrointestinal system. It is simple to locate idiopathic scoliosis patients with etiological models linking platelet calmodulin abnormalities, postural reflex problems in the brain, and gastrointestinal symptoms. The median and dorsal raphe nuclei of the brainstem contain serotonin neurons, which have projections to practically every region of the central nervous system. The pons and midbrain have serotonergic cell bodies that send descending axonal projections to almost all of the forebrain, regulating motor function and autonomic system activity.
Serotonergic pathways are important for postural control, and they target the thalamus, hypothalamus, cerebellum, and basal ganglia. Involuntary, reflexive control of posture is exemplified by the activation of fast-twitch antigravity muscle tone and the interpretation of horizontal and vertical from extra-ocular and vestibular structures. The CNS Body Schema, a central picture of normal postural representation, is generated and interpreted using postural input from the raphe nuclei. Using this image as a baseline, the CNS may maintain both static and dynamic postural equilibrium. As a consequence, sufficient serotonin synthesis is needed to maintain postural equilibrium.
Norepinephrine
Norepinephrine aids in the regulation of movement and muscle activity as a neurotransmitter. Compensatory physiological modifications, such as an increase in heart rate and blood pressure in reaction to stress or excitement, are the most common cause. Idiopathic scoliosis is a condition in which the spine twists abnormally due to dysfunction of the spinal cord. It occurs when norepinephrine levels are too high. There are a lot of norepinephrine pathways in the cerebellum, pons, and medulla. The norepinephrine cell bodies in these areas perform important functions of postural regulation, as well as autonomic management of visceral adaptation to postural alterations and dynamic equilibrium objectives.
Certain conditions, such as postural orthostatic tachycardia syndrome (POTS) and orthostatic hypotension, are often linked to abnormal norepinephrine output. Epinephrine, another important adrenal gland neurotransmitter involved in the stress response, is also produced from norepinephrine.
Drugs That Influence Neurotransmitters
Neurotransmitters are chemical messengers that aid in the communication between brain cells. Many medications, particularly those used to treat mental conditions, alter neurotransmitter levels. Selective serotonin reuptake inhibitors (SSRIs) slow the transport and absorption of serotonin by a neuron synapse, while Donepezil, galantamine, and rivastigmine stop the breakdown of acetylcholine inside one. Understanding drug abuse and addiction problems requires a knowledge of neurotransmitters’ function. It may also help explain why some individuals turn to a specific medication and why it is so difficult to quit.
Neurotransmitter Laboratory Testing
Direct neurotransmitter testing of the central nervous system can only be done by collecting cerebrospinal fluid. Because of the risks involved, peripheral urinary neurotransmitter collection is more clinically convenient, safer, and quicker than cerebrospinal fluid collection. Notwithstanding the fact that there is significant dispute over the veracity of direct neurotransmitter testing, peripheral measurements are frequently associated to diverse clinical symptoms and appearances.
Some facilities test urinary neurotransmitter metabolites, while others test direct urinary neurotransmitter levels. Despite the fact that there is considerable debate regarding clinical superiority between these two modalities, urinary neurotransmitter metabolites have the only disadvantage of being more difficult to study than catecholamine neurotransmitters.
Urine neurotransmitter levels, on the other hand, are readily assessed using enzyme-linked immunoassays (ELISA) and correlate to plasma levels. Urinary neurotransmitter tests may be beneficial clinical tools that aid physicians in the selection of effective treatment regimens with a positive therapeutic outcome. While they are not direct measurements of central nervous system levels, urinary concentrations of neurotransmitters do tend to correlate with circulating concentrations.
Treating Neurotransmitter Imbalances
Neurotransmitter imbalances may often be cured in a brief time period, particularly in cases when they are severe. Although there is no standard guideline for when clinicians should wait to re-test their patients, anecdotal evidence suggests a range of 8-12 weeks. Nutrient supplementation with over-the-counter pills may be a simple way to fix these imbalances from a functional medicine viewpoint. Dietary and/or lifestyle changes may be necessary in some cases as well.
Because neurotransmitter imbalances may be caused by a variety of different metabolic pathways, treatments for them may vary greatly.Treatment options can vary both by individual neurotransmitter imbalances (i.e. decreased or elevated) and abnormal ratios of neurotransmitters that are antagonistic to one another (i.e. serotonin and norepinephrine).
Dietary and Lifestyle Tips for Healthy Neurotransmitters
Restoring neurotransmitter levels may also be aided by dietary change. Many nutrients include an enzyme that helps the body make neurotransmitters on its own. Many animal and plant proteins contain a lot of serotonergic precursor amino acids. Other foods that may help to increase serotonin levels include dark chocolate and coconut. Some dietetic foods that may help increase norepinephrine include green tea, black licorice, and plant-based proteins. Some foods that may help reduce norepinephrine levels include chamomile tea, flax seed, chia seeds, and cruciferous vegetables. Some of the foods that contain high levels of bromelain and quercetin include pienapple, red grapes, berries, apples, red onions, raw broccoli, and green tea.
Clinical Significance
The brain’s neurotransmitters are crucial actors. They are chemical messengers that aid neurons share information. A variety of illnesses, disorders, and symptoms have been linked to neurotransmitter dysfunction. To raise neurotransmitter levels, there are natural treatment options available. Call us today to schedule your FREE scoliosis phone review, at 810-694-3576. You can also check out Dr. Morningstar’s podcast, Scoliosis World, for more information on neurotransmitters and scoliosis.